Finding the Best Pain Relief for Arthritis Proven Strategies

When you're trying to figure out the best pain relief for arthritis, it usually comes down to a smart mix of targeted topical treatments, simple lifestyle changes, and the right medical support. The most effective game plan is a personalized toolkit—one that combines fast-acting solutions like topical analgesics with long-term strategies to protect your joints.
Your First Step to Effective Arthritis Pain Management
Trying to navigate the world of arthritis relief can feel overwhelming, but the basic idea is pretty simple. Real, lasting comfort doesn’t come from a single magic bullet. It’s all about building a multi-layered defence system that’s tailored to your body, your lifestyle, and your specific kind of joint pain. Think of it less like finding one perfect solution and more like assembling a team of specialists who all work together.
This guide is your roadmap. We're cutting through the noise to focus on what actually works and exploring how different strategies can complement each other to create a powerful pain management system. The goal is to put you in control, helping you move from just reacting to pain to proactively managing your joint health.
The Three Pillars of Arthritis Relief
A solid pain management plan almost always rests on three core pillars that work in harmony. When you understand how each one contributes, you can build a more resilient and effective routine for better comfort and mobility every day.
This diagram shows how a complete approach to arthritis relief is built around these key areas.
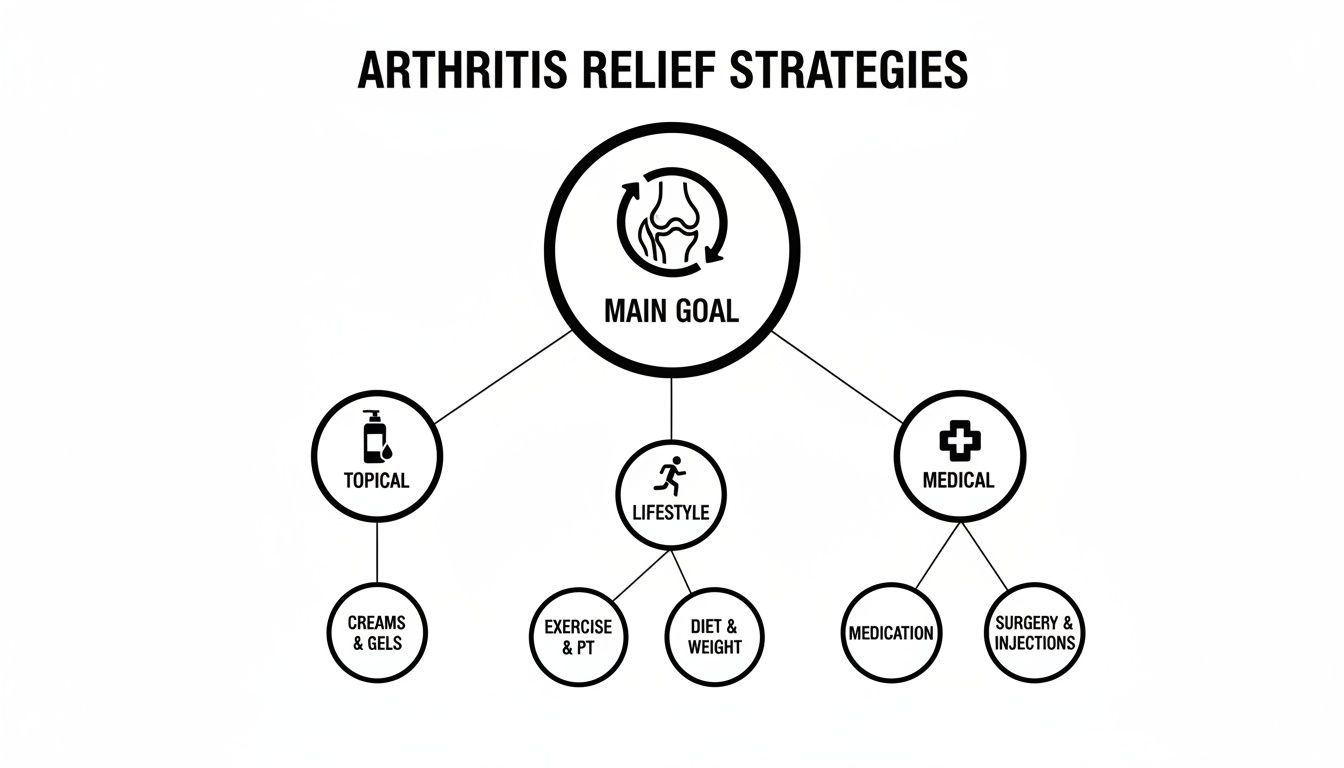
As you can see, the main goal—joint health—is supported by a balanced trio: direct topical treatments, foundational lifestyle habits, and necessary medical interventions.
To make this clearer, let's break down how these different methods stack up.
Quick Overview of Arthritis Pain Relief Methods
| Relief Type | Primary Mechanism | Best For | Example |
|---|---|---|---|
| Topical | Targets pain locally at the source with active ingredients | Quick, targeted relief for specific joints; pre/post-activity | Creams, gels, or sprays with menthol or methyl salicylate |
| Lifestyle | Reduces overall inflammation and strengthens joint support | Long-term management and improving overall joint health | Gentle exercise, weight management, anti-inflammatory diet |
| Medical | Manages systemic inflammation and disease progression | Moderate to severe arthritis; addressing underlying causes | Prescription medications, physical therapy, specialist care |
Each pillar plays a unique role, and the most effective strategies often involve combining elements from all three categories for comprehensive relief.
Understanding the Scope of Arthritis in Canada
The search for effective pain relief is a daily reality for millions. Here in Canada, arthritis affects over 6 million people, making it the number one cause of disability.
For many, it’s a major disruption to daily life. In fact, more than 40% of Canadians with arthritis say their pain is severe enough to limit their normal activities. This is why non-prescription options are so vital—people with arthritis are four times more likely to have pain interfere with their routines compared to those without the condition. You can find more insights about arthritis in Canada from the Arthritis Society.
By combining direct relief with supportive habits, you create a system where each part strengthens the others. A topical analgesic can ease pain enough to make gentle exercise possible, and that exercise, in turn, strengthens muscles to better support the joint long-term.
This integrated approach is the key to not just managing pain, but genuinely improving your quality of life. It’s about building momentum, where each small win makes the next one a little bit easier. From fast-acting topicals like MEDISTIK to sustainable, joint-friendly habits, every piece of the puzzle plays a crucial role.
Why Your Joints Hurt: Understanding Arthritis Pain
To really get a handle on arthritis pain relief, it helps to know what you’re up against. Figuring out what’s actually happening inside your joints is the first step toward a treatment that hits the true source of your discomfort, not just one that masks the symptoms. It’s all about getting to the root of the problem.
Think of your joint as a perfectly oiled door hinge, built to swing smoothly and quietly. Arthritis is what happens when that hinge starts to get rusty, stiff, and begins to grind. This breakdown can happen for a couple of different reasons, but the result is almost always the same: pain, stiffness, and trouble moving like you used to.
The two biggest players in the joint pain game are osteoarthritis and rheumatoid arthritis. They might both cause your joints to ache, but they come from completely different starting points.
Osteoarthritis: The “Wear and Tear” Process
Osteoarthritis (OA) is by far the most common type of arthritis, often called a "wear and tear" condition. Picture the cartilage in your joints like the thick, protective tread on a brand-new tire. After years on the road, that tread naturally wears down.
In your joints, cartilage is the smooth, slick tissue that cushions the ends of your bones, letting them glide over each other without a hitch. With OA, this cartilage gradually thins out and gets rough. If it wears down enough, it can disappear completely, leaving your bones to rub directly against each other.
That bone-on-bone grinding is what causes the deep, aching pain and stiffness that are the hallmarks of osteoarthritis. It’s like that door hinge losing its protective coating and grinding metal on metal. Your body might even try to fix the damage by growing little bony spurs, which can unfortunately make the pain and stiffness even worse.
Rheumatoid Arthritis: An Internal Attack
Rheumatoid arthritis (RA) is a whole different beast. It isn’t caused by years of mechanical use, but by an internal mix-up in your body’s own defence system. RA is an autoimmune disease, which means your immune system gets confused and starts attacking your own healthy tissues by mistake.
In this case, the immune system sets its sights on the synovium, the delicate lining inside your joints. You can think of the synovium as the built-in lubrication system that keeps the hinge moving freely. When it gets attacked, it becomes inflamed, swollen, and very painful.
This ongoing inflammation can eventually chew away at the cartilage and even the bone within the joint, leading to serious pain, deformed joints, and a major loss of function. Unlike OA, the pain from RA is driven primarily by this inflammatory fire, not just by friction.
The key takeaway is simple: Osteoarthritis pain comes from mechanical breakdown and friction, while rheumatoid arthritis pain comes from inflammation caused by an internal immune response. Understanding this distinction is crucial for finding effective relief.
No matter which type you’re dealing with, the pain can throw a wrench into your daily life. Something as simple as brushing your hair can feel impossible with shoulder arthritis, and stiffness in your legs can make every step a challenge. To see how arthritis can show up in different areas, you can learn more about symptoms and conditions like arthritis in the feet.
By figuring out if your pain is coming more from inflammation or from cartilage breakdown, you can choose strategies that tackle the problem head-on. This knowledge gives you the power to find the best pain relief for your specific kind of arthritis.
How Topical Pain Relievers Target Arthritis
Topical analgesics are a go-to strategy for a reason—they deliver relief exactly where you need it most. Picture it like sending reinforcements straight to the battleground of your sore joints instead of routing them through a long, complex supply chain. When you apply them directly to the skin, their powerful active ingredients get to work right at the source of the pain.
This targeted approach means the ingredients completely bypass your digestive system. That’s a huge plus, as it helps you avoid the systemic side effects, like stomach upset, that can sometimes tag along with oral pain pills. It's a smarter, more direct way to manage joint pain.

This kind of localized action is incredibly important, especially when you look at the sheer scale of arthritis in Canada. We’re talking about 6 million people affected and an annual economic hit of $33 billion. That’s a massive need for effective, easy-to-access solutions.
Innovations like Health Canada-approved MEDISTIK offer crucial non-prescription help, particularly for the 58% of people with arthritis who are under 65. As our population ages and joint replacements keep rising, the demand for powerful topicals that manage pain without surgery is only getting stronger. You can discover more insights about Canada's arthritis burden and its impact.
The Science Of Skin-Deep Relief
So, how does a simple cream or spray actually stop deep joint pain in its tracks? It all comes down to the active ingredients and how they interact with your body’s pain-signalling system. Different ingredients use distinct methods to provide relief, and many of the best formulas combine them for a multi-pronged attack.
Here are the main ways topical analgesics work their magic:
- Creating Counterirritation: Ingredients like menthol and camphor are known as counterirritants. They create a cooling or warming feeling on your skin that basically distracts your brain. Your nerves get busy processing these new sensations, which helps override and block the underlying pain signals coming from your arthritic joint.
- Reducing Inflammation: Salicylates, such as methyl salicylate, are chemically related to aspirin. Once absorbed through the skin, they work to slow down the production of prostaglandins—compounds that are key players in the inflammation process. This helps reduce both swelling and pain deep inside the tissue.
- Blocking Pain Signals: Certain ingredients act as local anesthetics, temporarily numbing the nerve endings in the skin. This stops them from sending pain signals to the brain in the first place, offering a more direct block against discomfort.
Understanding these different actions helps you see how a well-formulated topical provides more than just a surface-level sensation. It actively gets in the way of the pain and inflammation cycle, right where it’s happening. For a deeper dive, you can learn more about the benefits of a topical pain reliever versus an oral one.
A Multi-Ingredient System For Complete Care
While single-ingredient products can be useful, formulas that blend multiple active ingredients often deliver more complete and powerful relief. Why? Because they can tackle the pain from several angles at once. A product that contains both a counterirritant and an anti-inflammatory ingredient offers a potent one-two punch.
You get the immediate, fast-acting relief from the cooling or warming sensation, which helps you feel better right away. At the same time, the anti-inflammatory ingredients are working behind the scenes to address the underlying swelling and irritation for longer-lasting comfort.
This is exactly the approach MEDISTIK takes. Our extra-strength, multi-ingredient formulas are designed to work as a complete system. They don’t just mask the pain; they provide fast-acting relief with counterirritants while also delivering anti-inflammatory agents to tackle the source. It’s a powerful, non-prescription strategy trusted by over 10,000 clinics and even the Canadian Armed Forces.
This dual-action approach is what makes it such a great choice for everything from pre-activity warm-ups to post-activity recovery, helping you manage your arthritis pain and stay active.
Exploring Oral Medications and Medical Treatments
While topical analgesics offer powerful, targeted relief right where you need it, they are just one part of a complete pain management plan. For many people, the best approach to arthritis pain involves combining these localized treatments with systemic options like oral medications. This tag-team strategy helps manage pain from all angles, especially during those really tough flare-ups.
Oral medications work from the inside out. When you take a pill, it dissolves and enters your bloodstream, travelling throughout your entire body to do its job. It’s a completely different game plan from a topical, which sends its active ingredients straight through the skin to the painful joint.

Over-The-Counter Oral Pain Relievers
The most common starting point for oral arthritis relief is usually found right at your local pharmacy. These medications are generally effective for mild to moderate pain and you don't need a prescription to get them.
There are two main players in this category:
-
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): This group includes familiar names like ibuprofen and naproxen. NSAIDs work by blocking the enzymes that produce prostaglandins—the compounds that trigger both pain and inflammation. By tamping down inflammation system-wide, they can help ease joint swelling and discomfort.
-
Acetaminophen: Unlike NSAIDs, acetaminophen works primarily on the parts of the brain that register pain. It's a great pain reliever but doesn't have the same strong anti-inflammatory punch as NSAIDs, making it a different kind of tool for your arthritis toolkit.
It's important to understand the trade-offs here. While effective, long-term or high-dose use of oral NSAIDs can come with risks, including stomach irritation and potential kidney or heart issues. Always follow the package directions and have a chat with your pharmacist if you have questions.
This is where a combined approach really shines. Using a topical analgesic like MEDISTIK can give you powerful, direct relief, which might mean you don't have to rely as heavily on oral medications for every single ache. You can explore the science behind MEDISTIK’s powerful formulas to learn more.
When Your Doctor Steps In With Prescription Options
If over-the-counter options just aren't cutting it, or if you're dealing with a more severe or inflammatory type of arthritis like rheumatoid arthritis, your doctor has a whole range of stronger treatments up their sleeve. These prescription meds are designed to tackle more aggressive pain and disease progression head-on.
A healthcare professional might recommend several types of prescription treatments, depending on your specific condition and needs.
- Prescription-Strength NSAIDs: These are essentially more potent versions of their over-the-counter cousins. They offer stronger anti-inflammatory effects but require medical supervision because of a higher risk of side effects.
- Corticosteroids: These are powerful anti-inflammatory drugs, like prednisone, that can be taken as a pill or injected directly into a painful joint. They’re fantastic for calming down severe flare-ups but are usually only used for short periods due to potential long-term side effects.
- Disease-Modifying Antirheumatic Drugs (DMARDs): Used mostly for inflammatory conditions like rheumatoid arthritis, DMARDs work by reining in the body's overactive immune system. The goal is to slow down the disease itself and prevent permanent joint damage.
Creating a Cohesive Treatment Plan
The ultimate goal is to build a smart, sustainable plan that puts you back in control of your pain. Oral medications, whether from the pharmacy shelf or your doctor, can be foundational pieces of that plan, especially for managing systemic inflammation and severe pain.
But they don’t have to do all the heavy lifting. By adding a high-quality topical like MEDISTIK to your routine, you gain a powerful tool for on-the-spot relief. This complementary approach lets you tackle immediate, localized pain effectively while your systemic medications work on the bigger picture, helping you stay active and comfortable. Always talk to your doctor or pharmacist to make sure your combination of treatments is safe and effective for you.
Lifestyle Habits That Fight Arthritis Pain
While medication and topical treatments are fantastic tools, the most effective arthritis pain relief comes from a well-rounded strategy that includes your daily habits. The choices you make every single day can have a huge impact on your pain levels and the long-term health of your joints. These lifestyle adjustments work hand-in-hand with your treatments, building a stronger foundation for comfort and mobility.
Think of it like this: treatments manage the fire (the immediate symptoms), while your daily habits work on fireproofing the house (improving the underlying conditions). They're the proactive, long-term investments you make in your body. Simple changes to how you move, what you eat, and how you manage your weight can bring about some pretty significant and lasting results.
This approach is so important, especially when you consider how many people are affected. In Canada, 1 in 6 people live with arthritis, and a whopping 60% of them are of working age. It’s a huge issue, and finding practical, everyday strategies is key to maintaining a good quality of life.
Embrace Low-Impact Movement
When your joints are screaming, the last thing you probably feel like doing is getting up and moving. But here’s the thing: the right kind of movement is one of the best non-medical treatments for arthritis pain. Gentle, low-impact exercise is like pouring lubricant on stiff, creaky joints.
This kind of activity strengthens the muscles that surround your joints, which gives them much-needed support and stability. Think of these muscles as shock absorbers for your body—the stronger they are, the less stress gets put directly on your cartilage.
Try adding some of these activities to your weekly routine:
- Swimming or water aerobics: The magic of buoyancy! The water supports your body weight, taking the load off your joints while you build strength.
- Gentle yoga or tai chi: These practices are amazing for improving flexibility, balance, and your range of motion, all through slow, controlled movements.
- Cycling: Whether you’re on a stationary bike or hitting the trails, cycling is a fantastic low-impact way to boost your heart health and build leg strength.
Fuel Your Body with an Anti-Inflammatory Diet
The food on your plate can either fan the flames of inflammation or help to calm them down. An anti-inflammatory diet isn't about restriction; it's about focusing on whole foods packed with nutrients that fight inflammation from the inside out. It really comes down to making smart, simple swaps.
Focus on getting more of these foods into your meals:
- Fatty fish like salmon and mackerel (they're loaded with omega-3 fatty acids)
- Leafy greens like spinach and kale
- Nuts and seeds, especially walnuts and flaxseeds
- Berries and cherries, which are full of powerful antioxidants
- Olive oil as your go-to cooking fat
At the same time, it’s a good idea to limit processed foods, sugary drinks, and red meat, as they can all contribute to inflammation. On a related note, exploring various types of massage therapy can be a wonderful complementary strategy to help manage both inflammation and muscle tension.
Manage Your Weight to Reduce Joint Strain
Taking care of your weight-bearing joints—especially your knees, hips, and back—starts with managing your body weight. For every extra pound you carry, you're putting about four extra pounds of pressure on your knees. That adds up quickly.
Losing even a small amount of weight can lead to a significant reduction in pain and a major improvement in joint function. This isn't about hitting a specific number on the scale; it's about reducing the daily physical load on your joints.
The most effective game plan is combining a balanced, anti-inflammatory diet with regular low-impact exercise. This holistic approach doesn't just ease your current pain; it helps protect your joints from further damage, becoming a cornerstone of your long-term wellness. To layer in more effective habits, you can discover how to improve pain relief and recovery with complementary strategies.
Here’s a quick-glance table to help you put these lifestyle changes into action.
Joint-Friendly Lifestyle Changes for Arthritis Relief
| Strategy | Primary Benefit | Simple Actionable Tip |
|---|---|---|
| Low-Impact Exercise | Strengthens supporting muscles, improves joint lubrication and flexibility. | Start with a 15-minute walk or swim, three times a week, and gradually increase duration. |
| Anti-Inflammatory Diet | Reduces systemic inflammation that contributes to joint pain and swelling. | Swap one processed snack per day for a handful of walnuts or a bowl of berries. |
| Weight Management | Decreases the direct load and stress placed on weight-bearing joints like knees and hips. | Focus on portion control and aim to fill half your plate with vegetables at every meal. |
These small, consistent changes really do compound over time, making a big difference in how your joints feel day-to-day.
Knowing When to Consult a Doctor for Joint Pain
Taking charge of your arthritis pain with over-the-counter options and smart lifestyle choices is a fantastic way to stay in control of your health. But the best self-care plan always includes knowing when to tag in a professional. Think of your doctor not as a last resort, but as your most important teammate on your long-term joint health journey.
While you can often manage daily aches and stiffness at home, some symptoms are red flags that something more serious might be going on. Ignoring these signals can lead to worse pain or even permanent joint damage. It's so important to listen to what your body is trying to tell you.

Key Signs It Is Time for a Professional Opinion
Sometimes, joint pain is more than just an ache. Certain symptoms really need a prompt visit to your doctor for an accurate diagnosis and a more targeted treatment plan. Getting a professional look ensures you're on the right path and not just covering up a problem that needs specific medical attention.
Here are a few clear signs that it’s time to book an appointment:
- Sudden and Severe Pain or Swelling: If a joint flares up with intense pain, swelling, redness, or feels warm to the touch without any obvious injury, it needs to be checked out right away.
- Pain Accompanied by Systemic Symptoms: Joint pain that shows up with a fever, unexplained weight loss, or crushing fatigue is a major warning sign. It could point to an underlying inflammatory condition that needs addressing.
- Pain That Disrupts Your Sleep: Is your joint pain so bad that it consistently wakes you up at night or keeps you from getting a decent rest? That’s a clear signal your current management plan isn’t cutting it anymore.
- Limited Range of Motion: When you start struggling with simple daily tasks—like brushing your hair, tying your shoes, or reaching for a plate in the cupboard—because of joint stiffness or pain, it's time for a professional evaluation.
Getting a diagnosis isn't about losing control; it's about gaining clarity. A doctor can perform a physical exam, ask the right questions, and maybe use an X-ray to see what’s really happening inside the joint. This helps rule out other issues and confirms what's causing your pain.
When Your Current Plan Stops Working
Another key moment to see a doctor is when your go-to pain relief methods just aren't working like they used to. Maybe the topical analgesic that was your hero now barely takes the edge off, or your symptoms are slowly getting worse despite your best efforts with exercise and diet. This shift often means your condition is progressing and might require a new strategy.
A doctor can help you pivot. They might introduce prescription medications, recommend formal physical therapy, or talk about other medical options. Finding the best pain relief for arthritis isn't a one-and-done deal; it's a process. A professional provides the expert guidance you need to adapt your plan as your body changes, making sure you can keep managing your pain and living your life to the fullest.
Common Questions About Arthritis Pain Relief
When you're trying to manage arthritis pain, a lot of questions come up. Getting clear, practical answers is the first step toward building a relief strategy that actually works for you and that you can feel good about.
Let's dive into some of the most common questions we hear. Understanding how different treatments can work together, how quickly you can expect to feel better, and when to grab a hot or cold pack can make a huge difference in your daily comfort.
Can I Combine Topical Relievers with Oral Medications?
Yes, you absolutely can, and it's a very common and effective way to manage arthritis pain. Think of it as a two-pronged attack. A topical analgesic like MEDISTIK works locally—right on the surface where you apply it—targeting pain at the source without really entering your bloodstream.
Because it stays local, it almost never interferes with systemic oral medications like acetaminophen. This lets you tackle the pain from the outside-in and the inside-out for much better coverage. That said, it’s always a good idea to have a quick chat with your pharmacist or doctor before mixing a topical containing salicylates with an oral NSAID like ibuprofen. They can give you personalized advice to make sure you’re using everything safely.
How Quickly Do Topical Arthritis Products Work?
The answer really depends on the active ingredients in the formula. Products that contain counterirritants like menthol and camphor—the key ingredients in MEDISTIK's Spray or Roll-On—get to work almost immediately. They create a powerful cooling or warming sensation that essentially distracts your nerves from the pain, giving you very fast relief.
For a deeper, more sustained relief that also helps with inflammation, other formulas might take about 15-30 minutes to kick in fully.
The real secret to managing chronic pain with topicals is consistency. Using it regularly as directed is the key to getting the best, most lasting results and keeping pain levels down all day.
When you're consistent, you maintain a steady level of the active ingredients where you need them most, which leads to more reliable, ongoing relief from that persistent joint pain.
Is Heat or Cold More Effective for Arthritis Pain?
This is a great question! Both heat and cold therapy are fantastic tools, but they’re specialists. They each have a different job to do, so it's all about using the right one for the right situation.
-
Cold Therapy: This is your "calm down" treatment. It’s your go-to for acute flare-ups where you have sharp pain and obvious swelling. Cold constricts the blood vessels, which dials down inflammation and helps numb the area for immediate relief.
-
Heat Therapy: Think of this as your "loosen up" treatment. Heat is perfect for the chronic stiffness and dull, nagging aches that are so common with arthritis. It boosts blood flow, which helps relax tight muscles and soothe the entire joint.
Some of the more advanced topicals are actually designed to give you a unique cooling-then-heating sensation. This approach delivers the best of both worlds in one simple application—first calming the sharp pain, then relaxing the underlying stiffness.
For a powerful, non-prescription solution designed for warm-up, performance, and recovery, trust MEDISTIK. Our Health Canada-approved formulas provide targeted, extra-strength relief to help you manage arthritis pain and move with confidence. Explore the MEDISTIK system and find the right product for your needs.
 - LIVRAISON GRATUITE POUR LES COMMANDES $50+
- LIVRAISON GRATUITE POUR LES COMMANDES $50+

 - LIVRAISON GRATUITE DÈS 40 $ D’ACHAT
- LIVRAISON GRATUITE DÈS 40 $ D’ACHAT



